Vaccination against shingles in older people could have an unexpected benefit: reducing the chances of developing dementia. A study published this Wednesday in the prestigious journal Nature indicates that immunization against this virus is associated, over the following seven years, with a 20% reduction in the risk of developing this neurodegenerative disease.
The new results provide support for the hypothesis that certain infectious diseases can precipitate neurodegeneration. Advocates understand that certain preventive and therapeutic strategies, such as vaccines, antivirals, and antibiotics, may be useful against brain diseases.
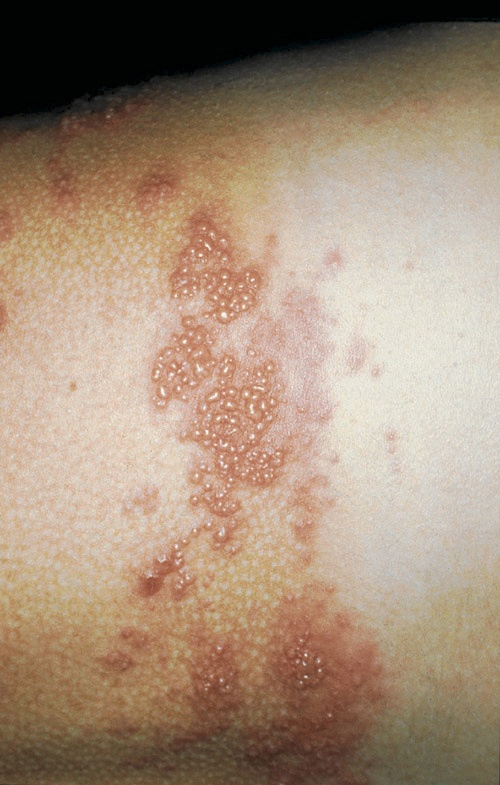
The virus that causes shingles, also colloquially known as herpes zoster, is the same as that of chickenpox. Once chickenpox is contracted, usually in childhood, the virus remains latent for life in nerve cells. In older people or those with weakened immune systems, the virus can reactivate and cause shingles.
What was the "natural experiment" about?
The research, according to the authors, leverages a "natural experiment" that occurred in Wales between 2013 and 2015 when shingles vaccination was introduced in certain age groups. The team led by Pascal Geldsetzer, associate professor of Medicine at Stanford University (California), analyzed the medical records of over 280,000 older adults aged between 71 and 88 who did not have dementia at the start of the vaccination program.
They focused their analysis on those who were closest to the vaccine eligibility threshold. Thus, individuals who turned 80 just before September 1, 2013, could not be vaccinated, while those who did so after that date could. This measure allowed comparing two population groups of very similar ages and characteristics, vaccinated and unvaccinated, over time, without the usual biases that plague this type of observational studies seeking associations.
By 2020, one in eight older adults, who by then were between 86 and 87 years old, had been diagnosed with dementia. However, among the vaccinated, a significant reduction in risk was observed.
Therefore, although previous studies based on medical databases had linked the herpes vaccine to a lower risk of dementia, it is known that vaccinated individuals are more engaged in health care and generally have different lifestyles compared to the unvaccinated in terms of diet and exercise.
Pascual Sánchez Juan, scientific director of the Center for Research of Neurological Diseases (CIEN) and spokesperson for the Spanish Society of Neurology (SEN), highlights that the article has generated a lot of interest in the scientific community since it was published two years ago as a preprint, before its appearance in the journal and peer review: "A 20% relative reduction in the risk of dementia is a striking figure; currently, we do not have any therapeutic tool that achieves this. If confirmed, this public health measure should be seriously considered," emphasizes the expert.
Despite its high prevalence, the search for effective treatments against dementia is proving elusive. For this reason, Sánchez Juan applauds the study's high methodological quality: "The results are quite solid, and it is difficult to think that they have been obtained by chance."
However, for now, he points out that although this study resembles a clinical trial in design, it is not one, and therefore a causal relationship cannot be established between vaccination and protection against dementia.
One of the most striking results was that the protective effect of prophylaxis was more pronounced in women, suggesting differences between sexes in immune response. Women produce more antibodies after vaccination, and at the same time, shingles is more common in them.
The possible relationship between infections and the onset of neurodegenerative diseases such as Alzheimer's and multiple sclerosis is an area of interest for researchers. Sánchez Juan points out that the hypothesis that certain pathogens may contribute to the development of dementia has gained strength in recent years, especially in the case of the herpes virus.
He explains that certain microbes can remain latent and upon reactivation, generate an inflammatory response that could contribute to neuronal damage. Thus, vaccination would help reduce the risk of dementia by preventing infections and the associated inflammatory response.
Research with a live virus vaccine
An important aspect of the study is that it was conducted with a live attenuated virus vaccine, withdrawn from the market in 2022. The adjuvanted recombinant vaccine available in Spain, designed from certain virus proteins, does not have the limitations of the previous one, contraindicated in immunocompromised patients due to the associated risk of infection or viral reactivation.
The researchers understand that the new vaccine, more effective against shingles, could have a similar or even superior impact to the previous one. However, Sánchez Juan warns that the results of this study cannot be extrapolated to the recombinant vaccine.
Stanford University reports that over the past two years, Geldsetzer's team has replicated the findings in Wales in other countries such as England, Australia, New Zealand, and Canada, which have implemented vaccination similarly.
Currently, the researchers state that they are seeking funding to conduct a randomized controlled clinical trial with a placebo to evaluate the effectiveness against dementia of a single injection of the live attenuated virus vaccine against herpes.